Trans Feminine Hormone Replacement Therapy
Time to read 15 mins
Introduction
Within this section of text, cross sex hormones for masculine to trans feminine and trans nonbinary individuals will be discussed. Medication’s will be divided into anti-androgens, used to suppress testosterone, and feminizing hormones such as estrogen and progesterone.
The goal of hormone therapy in MtF individuals is reducing the effects of testosterone and inducing feminine secondary sex characteristics. This can include but is not limited to →
Reversibility of changes is contingent on time spent on hormones along with what the desired change looking to be reversed is. Some changes are permanent.
Please consult a general practitioner if you wish to undergo hormone replacement therapy.
Effects
- Breast development
- Fat redistribution
- Reduction of body hair
- Changes to libido
- Softening of the skin
Anti-Androgens
Anti-androgens are primarily used to block the production of testosterone. The most commonly used anti-androgens are →
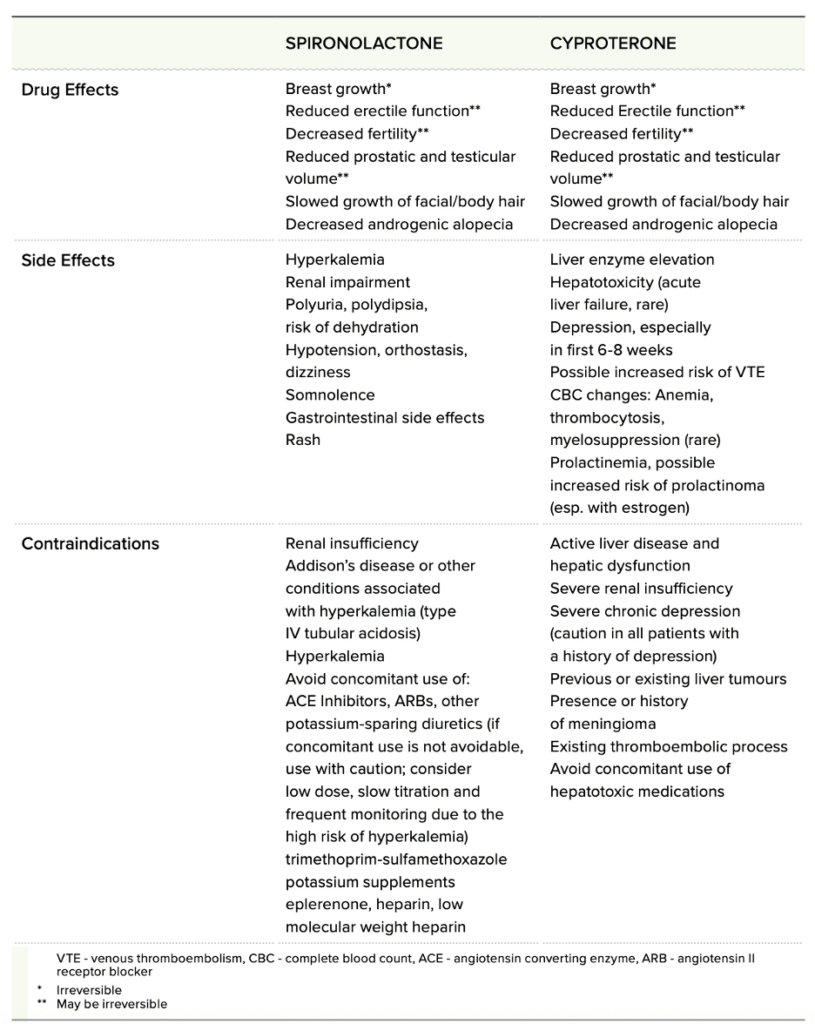
Spironolactone
Spironolactone is an orally taken potassium-sparing diuretic, meaning it helps your body get rid of extra water and sodium. At higher doses, it acts as an anti-androgen by blocking peripheral androgen receptors (Bourns et al., 2023 p. 38).
By blocking androgen receptors, testosterone will still be present in the bloodstream but will be unable to attach to receptors. This prevents its effects from triggering and can reduce →
(Bourns et al., 2023 p. 38)
Because testosterone levels do not significantly drop, patients should be hyper vigilant in monitoring their bodies for desired changes. Keeping a journal to document changes can be very helpful.
Changes are slow, and seeing results within a week or month is unlikely. While changes may begin within this timeframe, full effects and stability on spironolactone can take approximately 3–6 months (Bourns et al., 2023 p. 42).
Spironolactone is generally started at 50 mg taken daily and increased every 2–4 weeks if no negative side effects appear (Bourns et al., 2023 p. 40).
Because spironolactone raises potassium levels, it can be dangerous for patients with pre-existing kidney problems.
Spironolactone is covered by the Ontario Drug Benefit program without the need for an Exceptional Access Program and costs approximately $15–41 per month (Bourns et al., 2023 p. 40).
Additional Info
- Spironolactone
- Cyproterone
- Lupron (in some cases)
- Facial hair
- Spontaneous arousal
- Muscle growth
- Other masculinizing effects
Doses and Side Effects
- Typical effective dose: ~100 mg
- General maximum dose: 150 mg
- Absolute maximum dose: 300 mg
The main side effects to watch for include:
- Polyuria (excessive urination)
- Orthostasis (sudden drop in blood pressure when standing, causing dizziness or faintness)
- Erectile dysfunction
(Bourns et al., 2023 p. 42)
Cyproterone
Cyproterone is an oral synthetic steroid with progestin (synthetic progesterone) effects. It binds to androgen receptors, preventing testosterone from binding and masculinizing the body (Bourns et al., 2023 p. 38).
This can reduce →
Additionally, cyproterone has progestational activity and signals the brain to stop producing gonadotropins, the hormones responsible for telling the testicles to produce testosterone (Bourns et al., 2023 p. 38).
Because of this, cyproterone is considered a stronger anti-androgen than spironolactone, though this is based on clinical experience rather than large studies (Bourns et al., 2023 p. 38).
Effects
- Facial hair
- Spontaneous arousal
- Muscle growth
- Other masculinizing effects
Dose
- Starting dose: 12.5 mg
- Dose increases: 12.5 mg every 2–4 weeks
- Maximum dose: 50 mg
Side Effects
- Depression
- Low energy
- Erectile dysfunction
Lupron
Lupron is a less commonly used anti-androgen and is typically prescribed when a patient cannot tolerate spironolactone or cyproterone (Bourns et al., 2023 p. 41).
Lupron is an injectable gonadotropin-releasing hormone (GnRH). Normally, the brain releases GnRH to signal the pituitary gland to produce hormones. Lupron floods these receptors, briefly increasing hormone production before desensitizing the pituitary gland and stopping hormone signaling entirely (Bourns et al., 2023 p. 41).
At this point, the body produces almost no hormones.
Potential downsides of Lupron include →
The injection is intramuscular and typically administered in the thigh or buttock. Muscles may tense and cramp for several hours after injection.
Lupron is generally not covered by the Ontario Drug Benefit program.
Costs are approximately →
(Government of Ontario, Ministry of Health, n.d.)
Side Effects
- Permanent infertility with continuous use in patients assigned male at birth
- Anemia
- Fatigue
- Weight gain
- Hot flashes
- Decreased bone mineral density
- Loss of muscle mass
- Depression
- Memory loss
Dose
- 7.5 mg injected once monthly
- 22.5 mg injected once every three months
Costs
- $388 for a 7.5 mg injection
- $1159 for a 22.5 mg injection
Estrogen
Estrogens, which in this case refers to synthetic estrogens, interact with estrogen receptors in the body to initiate feminization (Bourns et al., 2023 p. 42).
Effects can vary greatly based on →
Estrogens are generally started 1–3 months after an anti-androgen is introduced. Unlike anti-androgens, many effects of estrogen are irreversible or require surgery (Bourns et al., 2023 p. 42).
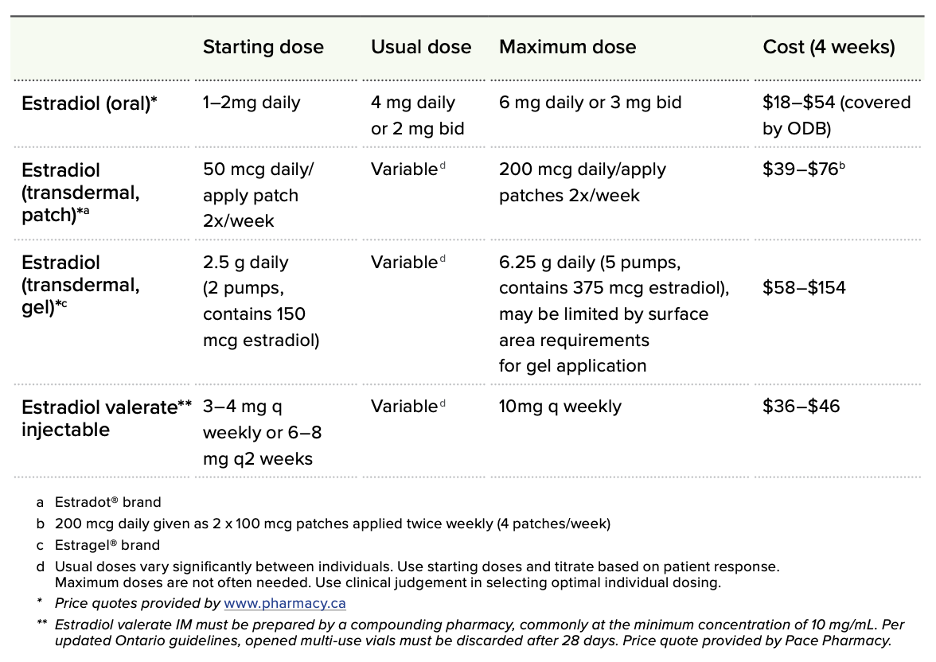
Estrogen is administered in one of three primary ways →
Considerations
- Age
- Genetics
- Body habits
- Dose and method of administration (to a lesser extent)
Types
- Orally (swallowed pill)
- Sublingually (pill dissolved under the tongue)
- Via injection
Progestins
Progestins are another feminizing hormone and are naturally produced during the second half of the menstrual cycle. Because of this, many trans-feminine people take progesterone, and there are many personal accounts of its effectiveness.
However, this contrasts with most studies, which have found no direct correlation between progesterone and breast growth or fat redistribution.
(Bourns et al., 2023 p. 46)
Progesterone is typically taken orally, where its effectiveness is reduced through metabolism before entering the bloodstream. It can also be taken transdermally via patch or cream, though this is almost exclusively when cyproterone is used as an anti-androgen (Szymczyk et al., 2024 p. 3).
Progesterone is a steroid hormone that binds to intracellular progesterone receptors and affects gene expression, causing some genes to turn on and others to turn off (Szymczyk et al., 2024 p. 2).
Because elevated progesterone levels occur in cis women before menstruation—when breasts may temporarily increase in size—some argue progesterone has similar effects in trans-feminine individuals. However, there is no scientific data supporting this.
Possible side effects of progesterone include →
The most common progestin is Prometrium (brand), taken orally at →
This is the preferred option because it is micronized and identical to progesterone produced in cis women.
Another option is Provera (brand), taken at doses ranging from 5–20 mg daily. This form is not identical, so doctors generally recommend Prometrium instead (Bourns et al., 2023 p. 47).
Progesterone is generally not covered by the Ontario Drug Benefit program unless accessed through the Exceptional Access Program. Costs are approximately →
Side Effects
- Weight gain
- Edema (excess fluid retention)
- Depression
- Increased risk of breast cancer
- Heart disease
- Stroke
- Venous thromboembolism
Dose
- 100MG
- 200MG
Costs
- $50 per month for 100 mg per day
- $100 per month for 200 mg per day
References
Vincent, B. (2018). Transgender health: a practitioner’s guide to binary and non-binary trans patient care. Jessica Kingsley Publishers.
Coleman, E., Radix, A. E., Bouman, W. P., Brown, G. R., de Vries, A. L. C., Deutsch, M. B., … Arcelus, J. (2022). Standards of Care for the Health of Transgender and Gender Diverse People, Version 8. International Journal of Transgender Health, 23(sup1), S1–S259.
Bourns, A., Edgar, A., Lou, A., Kucharski, E., Townsend, M., Fung, R., Hranilovic, S., Weisdorf, T., & Rainbow Health Ontario. (2023). Guidelines for gender-affirming primary care with trans and non-binary patients (4th ed., with 2023 updates) [PDF]. Sherbourne Health / Rainbow Health Ontario.
BC Cancer Agency. (2020, April 1). Leuprolide monograph [PDF]. BC Cancer.
Government of Ontario, Ministry of Health. (n.d.). Lupron Depot PDS (leuprolide acetate) — Formulary entry. Ontario Drug Benefit Formulary.
Szymczyk, S., Mączka, K., Mądrzak, L., Grymowicz, M., & Smolarczyk, R. (2024). The potential health risks and benefits of progesterone in the transgender woman population — A narrative review. Journal of Clinical Medicine, 13(22), 6795.
Government of Ontario. (n.d.). Check your medication coverage.
Government of Ontario. (n.d.). Formulary drug search: PMS-Progesterone.
